May is peak season for asthma and allergy symptoms, so it is a perfect time to raise awareness.
Asthma impacts 24.5 million Americans and more than 6 million children under the age of 18 suffer from asthma. Unfortunately, 10 people die every day from it.
Rates of allergies are increasing and now more than 50 million Americans have some type of allergy including pollen, skin, latex, and more. This makes allergies the 6th leading cause of chronic illness in the United States.
While there is no cure for asthma or allergies, there are many things we can do to control symptoms and decrease the number of preventable deaths.
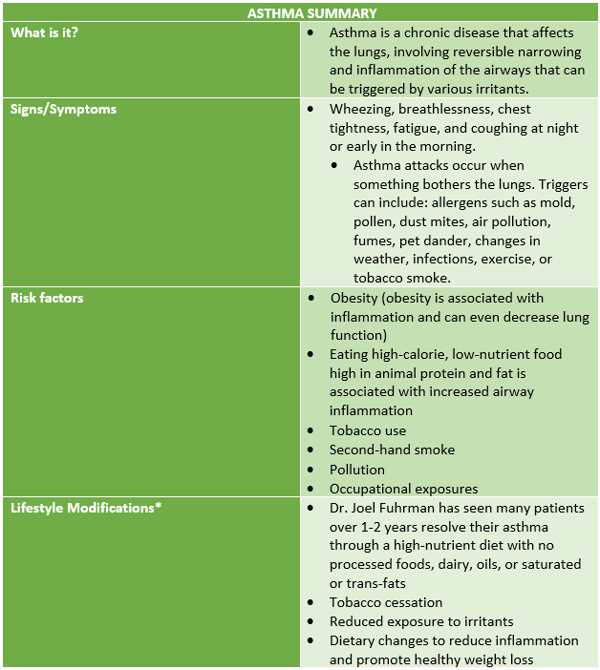
It can be difficult to know if you or your child has asthma. If you experience any of the symptoms listed above and you think you might have asthma, it’s important to talk to your doctor. They will likely ask you several questions about your symptoms and may do a breathing test to assess the function of your lungs.

The good news is that because asthma is a disease related to inflammation, there are a number of lifestyle changes that can impact it.
Dietary and environmental changes, as well as healthy weight loss, can significantly improve symptoms. Adopting an eating style that is nutrient-dense and anti-inflammatory can play a role in controlling symptoms.
Include good sources of quercetin such as berries (especially chokeberries and cranberries), citrus fruit, buckwheat, kale, watercress, red onion, black plums, among others, as they have anti-histamine and anti-inflammatory effects.
It is also helpful to include good sources of alpha-linoleic acid (ALA) including ground flax seeds, chia seeds, or walnuts to further reduce inflammation associated with asthma.
Environmentally, avoid tobacco and second-hand smoke as much as possible. Take all reasonable steps to decrease your exposure to common triggers such as pet dander, dust mites, and pollen.
Success Story: As a Medi-Share Health Coach and faithfully sharing member, Marcie knows first-hand the dramatic impact lifestyle changes can have on asthma. Just listen to this incredible interview with her:
Christian Care Ministry (CCM): When were you diagnosed with asthma?
Marcie (MG): I was diagnosed as an adult in my early 30s. I had issues with allergies for years that just kept getting worse and I would frequently get bronchitis… finally, I was diagnosed. I was told by the doctor that I had likely always had the asthma but something triggered it as an adult – perhaps after I had my first child or my move to a different state, or something else.
CCM: How did it impact your life?
MG: I am a distance runner, so this was not exciting news for me. I was put on daily prescription medications for the allergies and had to use an inhaler before I worked out, and also carry with me during runs. I did feel happy I could breathe again, but didn’t like hearing I’d have to do this for the rest of my life. I had always been thin and although I was eating the same, training, and completing half marathons regularly, I started gaining weight. I had never gained weight my entire life so I knew it was due to all the steroids that were daily going into my body.
CCM: What lifestyle changes did you make?
MG: I ate well by most people’s standards and because I was thin and ran a lot, I had the philosophy that I could really eat whatever I wanted. I started to get frustrated and started researching… up to this point I had just listened to my doctor and he prescribed meds, never mentioning how dietary changes could help. I started reading about different supplements, then was introduced to Dr. Fuhrman’s books and insights. I realized I had to make dietary changes to live the way I wanted to live. I had already cut out dairy, which is one of the first recommendations. I started adding in more vegetables, specifically cruciferous vegetables. I made sure I had cruciferous vegetables daily. I started eating walnuts or ground flaxseed daily and made big cutbacks on processed foods. Over time, I adapted all the suggestions Dr. Fuhrman had made. The changes slowly started kicking in and I went from prescription meds to just over the counter meds for the allergies, and inhaler use went down. Within just a few months I was off all meds and inhalers.
CCM: How long has it been since your last asthma symptom?
MG: More than 5 years.
CCM: How is your life different now?
MG: I love that I don’t have to put drugs in my body, love that I can sleep through the night without constant coughing, love that I don’t suffer from all the discomforts that come with allergies and asthma, and love that I can work out and run freely without having to worry about my breathing.
CCM: What are the key factors that prevent your asthma from returning?
MG: Without a doubt maintaining a nutrient-dense diet.
CCM: What advice do you have for those diagnosed with asthma?
MG: Eat a nutrient-dense diet… it’s tough to change your diet overnight, but it’s possible and the rewards are great. Cruciferous, cruciferous, every day!!!!!!
MG: Something else I’d like to share with you about my story: when I read “Disease Proof Your Child” (by Dr. Fuhrman), I realized the reason for my asthma came from how I ate as a kid. I was skinny and didn’t like to eat, so my parents let me eat what I wanted so as to maintain a healthy weight… which was a lot of carbohydrates. I could have lived on rice/cottage cheese/macaroni and cheese/ potatoes. I rarely ate fruit and vegetables! Also, my youngest son, who we adopted when he was two, had severe asthma. He had been hospitalized for it multiple times prior to us getting him and did nebulizer treatments twice daily. He was on a ton of stuff, and also had eczema. The first time he came to our house was the first time he had a vegetable. Long story short, within a month or two of living with us he was off all meds and breathing treatments. For him, I cut out dairy right away and fed him lots of fruits and vegetables. I also give him an omega 3 children’s supplement.
CCM: What an amazing success for both you and your son! Thank you for sharing!
*If you have been prescribed medications or inhalers, do not discontinue use without talking to your healthcare provider.
We can come into contact with allergens in multiple ways, as shown in this infographic from the Asthma and Allergy Foundation of America:

Conclusion
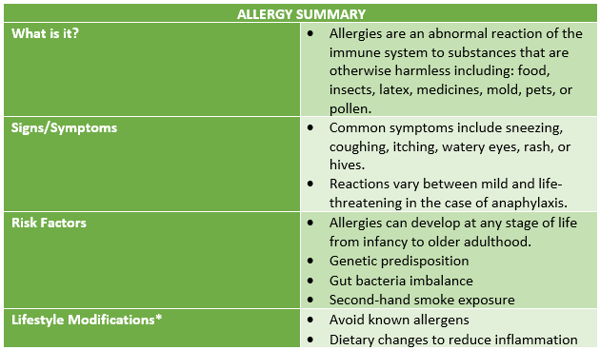
Talk to your doctor if you experience allergy signs or symptoms. You will likely be tested to identify your allergens.
Once allergens are identified, a treatment plan can be developed to keep allergies from interfering with your daily activities. Treatment options typically include avoidance of allergens, possibly medications, or immunotherapy which trains the immune system not to overreact to the allergen.
Once again, the fantastic news is that we have the power to impact allergies through our lifestyle choices. Of course, avoiding known allergens is important to minimizing symptoms, but that may not always be possible with insects and pollen outdoors and pets increasingly indoors, including in stores and airplanes.
Research indicates that populations that consume more plant-based foods have lower rates of allergies. Nutrient-dense plant foods provide the body the opportunity to allow the immune system to function properly which could lessen allergy symptoms naturally.
Consume a wide variety of vegetables, fruits, nuts, and seeds containing antioxidant and anti-inflammatory properties to reduce allergy symptoms. Some research shows higher rates of allergies in those that are Vitamin D deficient. Talk to your doctor and consider testing your Vitamin D levels. Supplementation with Vitamin D3 may be advised if your levels are low.
Show and teach your children to enjoy a healthy nutrient dense diet, encouraging their immune system to function properly right from the start.
Americans spend more than $18 billion a year on allergies and another $81.9 billion on asthma each year. For school-age children, asthma is one of the leading causes of missed school days.
It’s important for you and your healthcare provider to develop a comprehensive management plan. With these lifestyle changes, imagine the time, money, and headaches that could be saved across the nation by reducing symptoms of asthma and allergies.
Resources:
Anyo, G., Brunekreef, B., Meer, G. D., Aarts, F., Janssen, N. A., & Vliet, P. V. (2002). Early, current and past pet ownership: Associations with sensitization, bronchial responsiveness and allergic symptoms in school children. Clinical Experimental Allergy,32(3), 361-366. doi:10.1046/j.1365-2222.2002.01254.x
Asher, M. I., Stewart, A. W., Mallol, J., Montefort, S., Lai, C. K., Aït-Khaled, N., & Odhiambo, J. (2010). Which population level environmental factors are associated with asthma, rhinoconjunctivitis and eczema? Review of the ecological analyses of ISAAC Phase One. Respiratory Research,11(1). doi:10.1186/1465-9921-11-8
Asthma and Allergy Foundation of America. (2015, September). Allergies. Retrieved April 10, 2018, from http://www.aafa.org/page/allergies.aspx
Asthma and Allergy Foundation of America. (2018). May Is National Asthma and Allergy Awareness Month. Retrieved April 10, 2018, from http://www.aafa.org/page/asthma-and-allergy-awareness-month.aspx
Centers for Disease Control and Prevention. (2017, January 27). Asthma. Retrieved April 10, 2018, from https://www.cdc.gov/asthma/faqs.htm
Centers for Disease Control and Prevention. (2017, September 15). Gateway to Health Communication & Social Marketing Practice. Retrieved April 10, 2018, from https://www.cdc.gov/healthcommunication/toolstemplates/entertainmented/tips/Allergies.html
Frieri, M., & Valluri, A. (2011). Vitamin D deficiency as a risk factor for allergic disorders and immune mechanisms. Allergy and Asthma Proceedings,32(6), 438-444. doi:10.2500/aap.2011.32.3485
Fuhrman, J., MD. (n.d.). Allergies. Retrieved April 10, 2018, from https://www.drfuhrman.com/library/health-concerns/1/allergies
Fuhrman, J., MD. (n.d.). Asthma. Retrieved April 10, 2018, from https://www.drfuhrman.com/library/health-concerns/5/asthma
Kneepkens, C. M., & Brand, P. L. (2010). Clinical practice: Breastfeeding and the prevention of allergy. European Journal of Pediatrics,169(8), 911-917. doi:10.1007/s00431-010-1141-7
Matheson, M. C., Walters, E. H., Simpson, J. A., Wharton, C. L., Ponsonby, A., Johns, D. P., . . . Dharmage, S. C. (2009). Relevance of the hygiene hypothesis to early vs. late onset allergic rhinitis. Clinical & Experimental Allergy,39(3), 370-378. doi:10.1111/j.1365-2222.2008.03175.x
Wang, D. (2005). Risk factors of allergic rhinitis: Genetic or environmental? Therapeutics and Clinical Risk Management,1(2), 115-123. doi:10.2147/tcrm.1.2.115.62907





